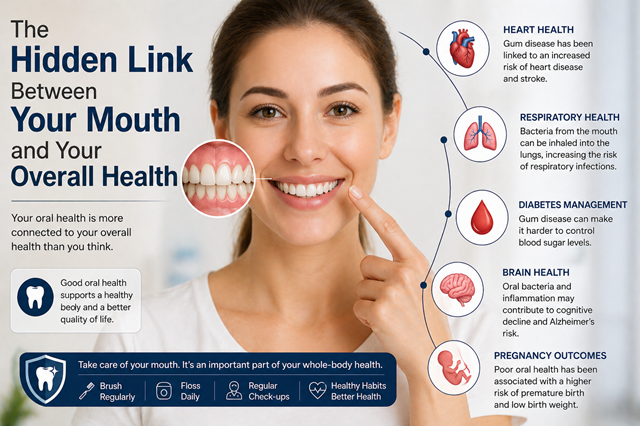
Oral health is often viewed as separate from general health, but the mouth is not an isolated system. It is directly connected to the rest of the body through blood flow, immune response, and bacterial activity. What happens in the mouth can influence conditions far beyond the teeth and gums.
At Georgian Mall Family Dental, preventive care is built on the understanding that oral health is closely linked to overall health. The goal is not to create alarm, but to provide education about how maintaining the mouth can support broader wellness outcomes over time.
The human mouth contains a complex ecosystem of bacteria. Many of these bacteria are harmless or beneficial when balanced properly. However, when oral hygiene is not maintained, harmful bacteria can increase in number and contribute to inflammation.
This inflammation does not always stay localized. In some cases, bacteria and inflammatory markers can enter the bloodstream through the gums, especially when gum tissue is compromised. Once in circulation, these factors may interact with other systems in the body.
This is one of the key reasons oral health is considered part of systemic health rather than a separate category.
Gum disease is one of the most well-studied conditions linking oral health to overall health. In its early stages, gum disease may present as mild inflammation or bleeding during brushing. In more advanced stages, it can affect the supporting structures of the teeth, including bone.
Chronic inflammation in the gums is not just a localized issue. It represents a long-term immune response that can place stress on the body. Research has explored connections between ongoing gum inflammation and broader inflammatory conditions in the body.
The important takeaway is not that gum disease directly causes systemic illness, but that it may contribute to inflammatory burden over time if left untreated.
One of the most widely discussed links in dental and medical research is the relationship between oral health and cardiovascular health. While the exact mechanisms are still being studied, inflammation appears to play a significant role.
When gum disease is present, bacteria and inflammatory markers can enter the bloodstream more easily. This may contribute to the formation of arterial plaque or increased strain on the cardiovascular system in some individuals.
It is important to approach this connection responsibly. Oral health is not the sole cause of heart conditions, but it is one of several contributing factors that may influence overall risk when combined with other health conditions such as diet, genetics, and lifestyle.
Diabetes and oral health have a bidirectional relationship. This means each can influence the other.
Individuals with diabetes are more likely to experience gum disease because elevated blood sugar levels can affect the body’s ability to manage bacteria and inflammation. At the same time, untreated gum disease can make it more difficult to maintain stable blood sugar levels.
This creates a cycle where each condition can potentially impact the other. For this reason, maintaining oral health is often considered an important part of overall diabetes management.
Preventive dental care helps reduce bacterial load and inflammation, which can support better overall stability for patients managing diabetes.
The mouth is also connected to the respiratory system. Bacteria from the oral cavity can be inhaled into the lungs, particularly in individuals with compromised immune systems or certain health conditions.
This is one reason why maintaining oral hygiene is especially important for older adults or individuals with existing respiratory conditions. Reducing bacterial buildup in the mouth may help lower the risk of respiratory complications in vulnerable populations.
Oral health is also closely linked to nutrition. The ability to chew comfortably affects dietary choices, which in turn influences overall health.
When dental issues such as decay, missing teeth, or gum discomfort are present, patients may avoid certain foods that are harder to chew. This can sometimes lead to reduced intake of nutrient-rich foods such as fruits, vegetables, and proteins.
Over time, these dietary adjustments can influence general health and energy levels. Maintaining oral function helps support a more balanced and varied diet.
One of the most important concepts connecting oral health and overall health is inflammation. Inflammation is a natural immune response, but when it becomes chronic, it can affect multiple systems in the body.
Oral inflammation, particularly from gum disease, can contribute to the body’s overall inflammatory load. While this does not directly cause systemic disease, it is one of several factors that researchers continue to study in relation to long-term health outcomes.
This is why preventive dental care is often framed not only as oral maintenance, but as part of broader health maintenance.
Preventive dentistry is not only about avoiding cavities or gum disease. It is about reducing risk factors that may influence overall health over time.
Regular dental visits allow for early detection of inflammation, infection, or structural changes in the mouth. When these issues are identified early, they can often be managed before they progress.
At Georgian Mall Family Dental, preventive care is approached with this broader perspective in mind. The goal is to support long-term stability, not only in oral health but in overall wellbeing.
One of the most important aspects of understanding the mouth-body connection is communication between dental and medical care. Patients who manage chronic conditions benefit from coordinated awareness of how oral health may interact with their overall health plan.
This does not mean dental professionals replace medical care. Instead, it highlights the importance of shared awareness between systems. When oral health is monitored consistently, it becomes easier to support overall health management in a more integrated way.
It is important to interpret the connection between oral health and systemic conditions responsibly. Oral health is not the sole cause of complex diseases such as heart disease or diabetes. These conditions are influenced by multiple factors including genetics, lifestyle, environment, and medical history.
However, oral health is one contributing factor that can be influenced through consistent preventive care. Maintaining healthy gums and teeth reduces bacterial load, supports lower inflammation levels, and contributes to overall wellness.
The focus should not be on fear or assumptions, but on informed awareness and preventive action.
One of the most effective ways to support both oral and overall health is early intervention. Identifying and treating oral conditions in their early stages reduces the likelihood of long-term complications.
Small areas of inflammation, early decay, or gum sensitivity can often be managed with relatively simple care when addressed promptly. When left untreated, these issues may progress and require more extensive treatment.
Early intervention supports not only dental outcomes but also reduces potential contributions to systemic stress over time.
Oral health is a key component of overall health maintenance. While it is only one part of a larger system, it plays a meaningful role in supporting long-term wellbeing.
By maintaining regular preventive care, patients reduce inflammation, manage bacterial balance, and support overall bodily health in a practical and ongoing way.
The connection between the mouth and the body is not theoretical. It is biological, measurable, and clinically relevant. Understanding this relationship helps patients make more informed decisions about their care and reinforces the value of prevention as a long-term health strategy.







Get all latest content delivered to your email a few times a month.
Resources: